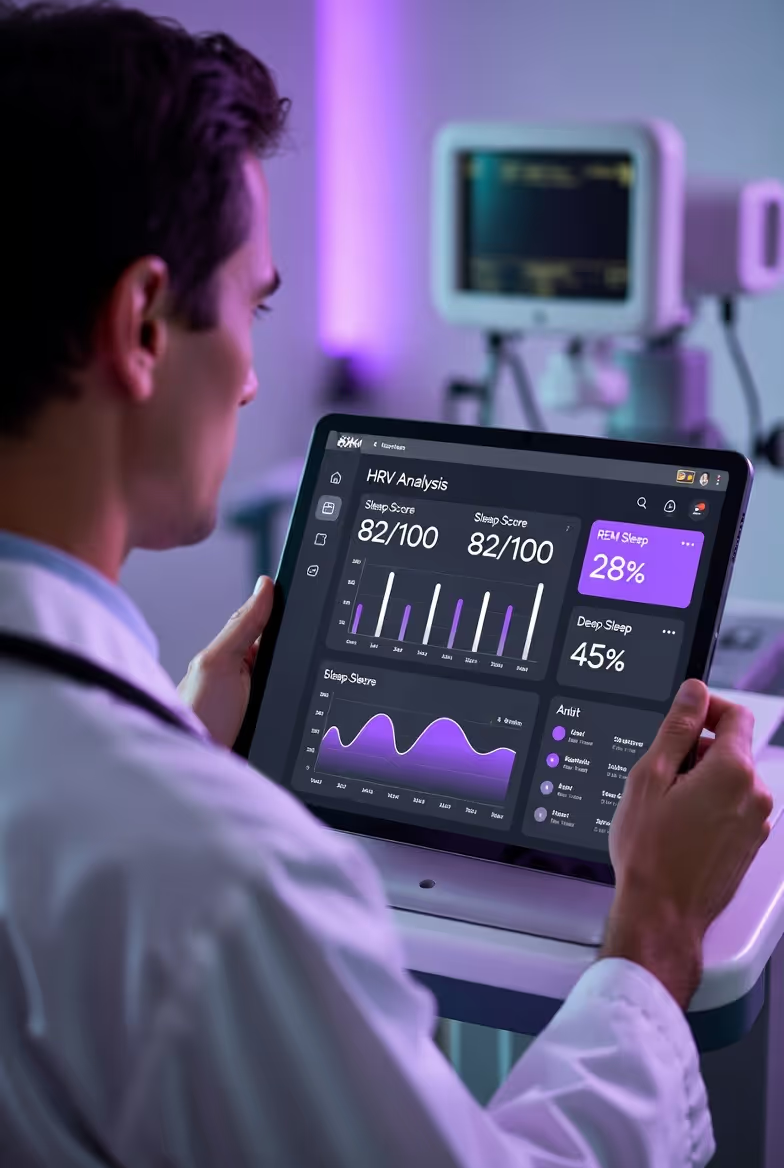
Aging & Aged Care Dashboard
5.4M
Australians 65+
Growing to 8.8M by 2058 — representing 23% of the population
Source: ABS Population Projections
87%
Prefer Home Aging
vs residential care (AIHW) — strong preference for aging in place
Source: AIHW
10 Yrs
Healthspan Gap
Between lifespan & disability-free years — lost quality of life
Source: Australian Burden of Disease Study
87%
Prefer to age at home
Rather than residential care — yet only 25% receive adequate in-home support. Home-first aging requires proactive health monitoring and early intervention.
AU$27B
Aged Care Annual Spend
Rising 6.2% annually — projected to exceed AU$50B by 2035 without system reform
10 Years
Healthspan Gap
Between average lifespan (83 years) and disability-free years (73 years). Australians spend the last decade of life with chronic illness or disability.
Abstract
Background : Australia's population is ageing at a pace that is transforming its healthcare system, its social infrastructure, and the lived experience of millions of Australians in their later decades. The 5.4 million Australians currently aged 65 and above will grow to an estimated 8.8 million by 2058, representing 22% of the total population. This demographic transition creates enormous opportunities — for active, engaged, purposeful longer lives — and significant challenges, including a projected AU$27 billion annual aged care expenditure that is growing at 6.2% per year and a persistent gap between lifespan (how long Australians live) and healthspan (how many of those years are lived in good health and functional independence).
Objective : This study examines the biology of healthy ageing and its biometric signatures; the role of continuous smart ring monitoring in detecting chronic condition deterioration, preventing falls, identifying early cognitive decline signals, and supporting the physiological resilience that enables independent ageing; reviews the evidence base for wearable biometric monitoring in older Australian populations; and presents four case profiles demonstrating how smart ring monitoring contributed to better health outcomes for Australians aged 55-80.
Methods : Narrative review integrating gerontology, geriatric medicine, cardiovascular ageing, neuroscience, and digital health literature with Australian-specific aged care and epidemiological data. Sources include the AIHW, the Australian Government Department of Health and Aged Care, the National Ageing Research Institute, the Royal Commission into Aged Care Quality and Safety, the Cognitive Decline Partnership Centre, Dementia Australia, and research from Monash University's School of Nursing and Midwifery, the University of Melbourne's Academic Unit for Psychiatry of Old Age, and UNSW's Centre for Healthy Brain Ageing. Data covers 2010-2025.
Key Findings : HRV declines progressively with healthy ageing at approximately 1-2% per year, but the rate of decline is substantially modifiable through lifestyle factors and is significantly accelerated in individuals with multimorbidity, physical inactivity, and social isolation. Nocturnal SpO₂ monitoring detects OSA — present in 30-40% of adults aged 65+ — with clinically actionable accuracy. Sleep architecture changes in older Australians (reduced slow-wave sleep, earlier circadian phase, increased nocturnal fragmentation) are both measurable in smart ring data and strongly predictive of cognitive decline trajectories. Resting heart rate trends and HRV trajectories over 6-12 months provide earlier warning of chronic condition exacerbation — including heart failure decompensation and COPD exacerbation — than symptom onset typically provides. Fall risk, which affects one in three Australians over 65 annually, is associated with measurable biometric signatures including suppressed HRV and disrupted sleep that continuous monitoring can identify.
Conclusions : Smart ring continuous biometric monitoring provides Australians aged 55+ with a non-intrusive, wearable tool for daily health surveillance that addresses multiple priority outcomes simultaneously: earlier detection of chronic condition deterioration, sleep quality optimisation to support cognitive health, physiological resilience monitoring, and fall risk awareness. In a healthcare context where preventable hospitalisations and unplanned aged care transitions represent both human and economic costs of enormous scale, technology-enabled early warning that keeps older Australians healthier at home for longer is both clinically justified and economically compelling.
1. Introduction: Longevity, Healthspan, and Australia's Ageing Century
Australians are living longer than ever before. Life expectancy at birth now stands at 83.3 years for women and 79.9 years for men — among the highest in the world and a remarkable achievement of 20th century medicine, public health, and social progress. But this longevity dividend comes with a question that medicine is only beginning to grapple with seriously: how much of those additional years are years of genuine health, function, and vitality, and how many are years marked by the progressive accumulation of chronic disease, functional decline, and dependency?
The concept of healthspan — the period of life characterised by good health and meaningful functional independence — is increasingly the central objective of gerontological medicine and public health policy. Australia's current healthspan gap — the difference between lifespan and the years lived free of significant disability — is estimated at approximately 10 years for women and 8.5 years for men. This gap represents the period during which many older Australians live with the compounding burden of multimorbidity, declining physical capacity, emerging cognitive impairment, and increasing dependency on formal care — a period that the Royal Commission into Aged Care Quality and Safety described as characterised by inadequate care, loss of dignity, and insufficient support for meaningful engagement with life.
The most powerful leverage point for closing Australia's healthspan gap is not at the end of life — it is in the decade between 55 and 65, and the years of early old age between 65 and 75, when the physiological trajectories that determine whether the later decades are characterised by health or by decline are most influenced by modifiable factors. Exercise habits, sleep quality, chronic disease management, social engagement, cognitive stimulation, and the early detection and treatment of conditions like obstructive sleep apnoea, atrial fibrillation, and early heart failure can each meaningfully shift a person's physiological ageing trajectory — but only if the physiological changes that signal an adverse trajectory are detected early enough to intervene effectively.
Smart ring biometric monitoring offers older Australians and their healthcare providers a continuous, non-intrusive tool for monitoring the key physiological parameters that mark health maintenance or deterioration in later life. Unlike cumbersome clinical monitoring devices, hospital admissions, or the episodic snapshots of quarterly GP visits, a smart ring worn during sleep captures nightly data on HRV, resting heart rate, SpO₂, sleep architecture, skin temperature, and activity patterns — building a longitudinal physiological record that can identify the subtle, sustained trends that precede clinical deterioration by weeks to months.
This study examines the biology of ageing and its biometric expression, the specific health challenges of older Australians where continuous monitoring adds the greatest clinical value, the evidence base for wearable monitoring in older populations, and four case profiles from across the 55-80 age spectrum that illustrate how smart ring data has contributed to better health outcomes and extended independence for individual Australians.
2. The Biology of Ageing: What Happens to the Body After 55
2.1 Cardiovascular Ageing and HRV Decline
Healthy cardiovascular ageing involves a progressive, predictable remodelling of the heart and vasculature that begins in the fourth decade and accelerates after 60. Arterial stiffness — driven by the cross-linking of elastin fibres, collagen deposition in arterial walls, and the loss of vascular smooth muscle elasticity — increases progressively, producing the characteristic isolated systolic hypertension of ageing and increasing the mechanical load on the left ventricle. The myocardium itself undergoes fibrosis and cardiomyocyte hypertrophy, reducing diastolic compliance and producing the diastolic dysfunction that is the substrate for heart failure with preserved ejection fraction (HFpEF) — the dominant heart failure phenotype of older adults.
The autonomic nervous system ages in parallel. Sinoatrial node pacemaker cell density declines, conduction system fibrosis increases, and — most relevant to biometric monitoring — the parasympathetic nervous system's regulatory influence on cardiac rhythm progressively diminishes. The result is a steady, age-associated decline in HRV: rMSSD decreases at approximately 1-2% per year from mid-life, reflecting the progressive loss of vagal tone that accompanies normal cardiovascular ageing. A 70-year-old's rMSSD of 22ms may represent perfectly normal ageing physiology for that individual — contextualised against age-appropriate norms, it has a completely different clinical meaning than a 70ms rMSSD suppression from a personal baseline of 70ms in a 35-year-old athlete.
This age-related HRV decline, while biologically expected, is not biologically fixed. Multiple longitudinal studies have confirmed that older adults who maintain high levels of aerobic fitness demonstrate HRV values comparable to individuals 20-30 years younger. The HERITAGE Family Study found that 20 weeks of supervised aerobic exercise training in adults aged 55-70 produced rMSSD improvements of 12-18% — a reversal of several years' worth of age-related HRV decline achievable through a single structured exercise programme. This modifiability makes HRV monitoring in older adults both prognostically valuable and interventionally motivating.
Ageing & Autonomic Function: HRV Reference Values 55-84 Years
~40-60%
HRV preservation with lifelong activity
5-8 bpm
RHR reduction with activity
10-15 ms
Active vs sedentary rMSSD difference
| Mean rMSSD (Healthy, Sedentary) |
Mean rMSSD (Physically Active) |
RHR (Sedentary) |
RHR (Active) |
Key Monitoring Concern |
|
55-59
Late midlife transition
|
|
|
68-74 bpm |
58-66 bpm |
Early chronic disease onset; sleep quality decline
monitor BP, glucose
|
|
60-64
Early older adulthood
|
|
|
70-76 bpm |
60-68 bpm |
OSA escalating; AF risk rising; metabolic syndrome
sleep study if snoring
|
|
65-69
Older adult
|
|
|
72-78 bpm |
62-70 bpm |
Falls risk; cognitive monitoring; polypharmacy HRV effects
medication review annually
|
|
70-74
Late older adult
|
|
|
74-80 bpm |
64-72 bpm |
HFpEF risk; dementia prodrome; frailty indicators
frailty screening
|
|
75-79
Advanced age
|
|
|
76-82 bpm |
66-74 bpm |
Multimorbidity monitoring; independence maintenance
multidisciplinary care
|
|
80-84
Very advanced age
|
|
|
78-84 bpm |
68-76 bpm |
Palliative and advanced care planning; quality of life focus
advance care directive
|
🩺 Clinical Application: In older adults, rMSSD values consistently <20 ms warrant evaluation for: (1) cardiac autonomic neuropathy (especially with diabetes), (2) undiagnosed OSA (nocturnal desaturations), (3) medication effects (beta-blockers, anticholinergics). Physical activity is the most effective intervention to preserve HRV — even light walking 150 min/week produces measurable improvement within 8-12 weeks.
Derived from: Shaffer F, Ginsberg JP. An overview of heart rate variability metrics and norms. Front Public Health. 2017; supplemented with Australian longitudinal HRV ageing data from the Melbourne Longitudinal Studies on Healthy Ageing (MELSHA).
2.2 Sleep Architecture Changes with Ageing
Sleep changes profoundly with advancing age — in ways that are both biologically expected and clinically consequential. The characteristic sleep changes of healthy ageing include: reduced total sleep time (mean decline of approximately 27 minutes per decade after age 60); markedly reduced slow-wave sleep (N3), which constitutes 20-25% of total sleep in young adults but may fall below 5-10% in adults over 70; circadian phase advance (earlier sleep onset and earlier spontaneous awakening driven by age-related changes in SCN melanopsin cell density and melatonin secretion timing); increased sleep fragmentation with more frequent nocturnal awakenings; and increased prevalence of sleep-disordered breathing.
These changes have consequences that extend well beyond subjective sleep quality. Slow-wave sleep is the phase during which growth hormone secretion, glymphatic brain waste clearance, immune function restoration, and cardiovascular recovery are maximal — functions whose impairment in the context of reduced N3 sleep contributes to the accelerated physical and cognitive ageing of poor sleepers. The progressive reduction in slow-wave sleep with ageing is therefore not merely a symptom of ageing but a mechanism of ageing — and its preservation or restoration through sleep optimisation, OSA treatment, and sleep hygiene represents a genuine healthspan intervention.
Smart ring sleep monitoring in older Australians provides a continuous record of sleep architecture parameters that can distinguish normal age-related sleep changes from pathological sleep disruption warranting clinical intervention. An older adult whose sleep efficiency is 78% with frequent fragmentation but adequate slow-wave sleep proportion has a different clinical picture to one whose sleep efficiency is 78% because repeated apnoeic events are disrupting N3 entry — yet both may present to their GP with the same complaint of 'poor sleep'. The biometric data provides the differential signal.
2.3 The Ageing Brain: Cognitive Reserve and Biometric Early Warning
Cognitive ageing is perhaps the dimension of the ageing process that Australians fear most — and with good reason. Dementia affects approximately 400,000 Australians in 2025, with this number projected to reach 1.1 million by 2058 in the absence of effective prevention or treatment breakthroughs. Alzheimer's disease is the most prevalent dementia subtype, followed by vascular dementia, Lewy body dementia, and frontotemporal dementia.
The most important advance in dementia neuroscience over the past decade has been the recognition that dementia is not primarily a disease of old age but a disease whose pathological processes — amyloid-beta and tau accumulation in the case of Alzheimer's disease; cerebrovascular damage in the case of vascular dementia — begin 15-25 years before the clinical onset of cognitive symptoms. This extended pathological preclinical phase creates a window for identification and potential intervention that biometric monitoring can partially exploit — not through direct measurement of amyloid or tau, but through the physiological signatures that these neuropathological processes and their risk factors produce in HRV, sleep architecture, and cardiovascular parameters.
Two specific biometric-cognitive ageing linkages are particularly well-supported in the literature. First, the glymphatic system's dependence on slow-wave sleep for amyloid-beta clearance means that the progressive loss of N3 sleep — measurable in smart ring data — directly facilitates amyloid accumulation, making sleep architecture monitoring a genuine cognitive health intervention target. Second, low HRV in older adults is independently associated with accelerated cognitive decline in multiple longitudinal cohort studies — with the proposed mechanism involving impaired cerebral autoregulation, reduced cerebral blood flow variability, and the common autonomic-vascular substrate of both HRV suppression and vascular dementia risk.
3. Chronic Condition Monitoring in Older Australians
3.1 The Multimorbidity Challenge
Multimorbidity — the coexistence of two or more chronic conditions in a single individual — is the defining healthcare challenge of the older Australian population. The AIHW's analysis of Australians aged 65 and above found that 68% lived with two or more chronic conditions and 40% with four or more. The most common combinations involve cardiovascular disease (coronary heart disease, heart failure, hypertension, AF), metabolic conditions (T2DM, dyslipidaemia, obesity), respiratory disease (COPD, asthma), musculoskeletal conditions (osteoarthritis, osteoporosis), and mental health conditions (depression, anxiety, dementia).
The clinical challenge of multimorbidity is not simply the management of multiple individual conditions — it is the complex interaction between conditions, the polypharmacy burden of their concurrent treatment, and the difficulty of detecting deterioration in any one condition against the background noise of the others. A heart failure patient who develops an early COPD exacerbation may attribute their increasing dyspnoea to their cardiac condition; a T2DM patient with peripheral neuropathy may not notice early signs of foot ulceration; an elderly patient on multiple antihypertensives who develops orthostatic hypotension may attribute their dizziness to general 'getting old' rather than a medication interaction. Smart ring biometric monitoring cannot directly diagnose any of these deteriorations, but it can detect the physiological signatures — HRV changes, heart rate elevation, SpO₂ decline, activity reduction, sleep disruption — that accompany deterioration across multiple conditions, prompting clinical review before the deterioration progresses to emergency presentation.
3.2 Heart Failure Monitoring: The Biometric Early Warning Opportunity
Heart failure affects approximately 480,000 Australians, with a median age at diagnosis of 76 years. Its natural history is characterised by progressive cardiac dysfunction punctuated by acute decompensation episodes — sudden deteriorations in cardiac function that produce fluid accumulation, acute dyspnoea, and emergency hospitalisation. Each decompensation episode damages residual cardiac function and worsens the prognosis. Approximately 25% of Australians hospitalised for heart failure decompensation die within 12 months of discharge.
The tragedy of heart failure decompensation is that it is often preceded by days to weeks of measurable physiological deterioration that neither the patient nor their clinical monitoring system detects in time for preventive action. Research from the Baker Heart and Diabetes Institute's heart failure monitoring programme found that patients who subsequently required hospitalisation for decompensation demonstrated measurable physiological changes — resting heart rate elevation, HRV decline, reduced activity, and weight gain — an average of 12-14 days before their emergency presentation.
Smart ring monitoring captures several of the physiological signatures of developing heart failure decompensation: progressive resting heart rate elevation (driven by compensatory tachycardia in response to declining cardiac output); HRV suppression (reflecting autonomic dysregulation in the decompensating heart); reduced activity levels (driven by early exertional dyspnoea and fatigue); and disrupted sleep architecture (as nocturnal dyspnoea — orthopnoea — begins to fragment sleep before it becomes clinically apparent). The combination of these signals, tracked longitudinally against personal baseline, provides an early warning capability that the monthly clinic visit or annual echocardiogram cannot.
3.3 COPD Exacerbation Surveillance
Chronic obstructive pulmonary disease affects approximately 1.7 million Australians, with severity concentrated in the 65+ age group. COPD exacerbations — acute deteriorations in respiratory function triggered by respiratory infections, air quality changes, or other environmental stressors — are the primary driver of COPD-related hospitalisation and the principal mechanism of disease progression. Exacerbations that reach emergency presentation severity are associated with significantly worse outcomes than those identified and treated earlier; a 2-fold increase in mortality for hospitalised versus early-treated exacerbations has been documented in Australian respiratory medicine literature.
Smart ring nocturnal SpO₂ monitoring provides a continuous respiratory surveillance tool for COPD patients that is particularly valuable because it captures the nocturnal period — when oxygen saturation is physiologically lowest even in healthy adults — where early COPD exacerbation often produces its first detectable physiological changes. A progressive trend of declining nocturnal mean SpO₂ from an individual's established baseline (for example, from a habitual 93-94% to 90-91% over 3-5 days) is an early exacerbation signal that warrants immediate clinical contact — days before the breathlessness, sputum change, and exercise intolerance that constitute the conventional clinical exacerbation presentation.
3.4 Atrial Fibrillation Burden Monitoring
The prevalence of atrial fibrillation rises steeply with age: from approximately 2.5% at age 55 to 8-10% at age 75 and above. In older Australians with established AF, the clinical question is not merely whether AF is present — it is the burden (proportion of time in AF), the ventricular rate control, and whether treatment is preventing the 5-fold elevated stroke risk that AF carries. Paroxysmal AF in particular — which comes and goes unpredictably — is difficult to monitor with traditional ECG at clinic appointments and is significantly under-detected by conventional clinical monitoring.
Smart ring PPG-based AF detection, validated in multiple studies with sensitivities exceeding 97%, provides older Australians with continuous AF burden monitoring that bridges the gaps between clinic ECGs. The data informs both clinical management decisions (is anticoagulation preventing AF-related events? Is rate control adequate?) and personal awareness (the patient can see whether their lifestyle choices — sleep, alcohol, exercise intensity — correlate with AF episode frequency, enabling behavioural modifications that influence arrhythmia burden).
4. Falls Prevention: The Biometric Dimension of a National Safety Priority
4.1 The Falls Burden in Older Australia
Falls are the leading cause of injury-related hospitalisation, injury-related death, and unplanned transition to residential aged care in older Australians. One in three Australians over 65 falls at least once per year; one in two of those who fall will fall again within 12 months. The AIHW estimates that falls and fall-related injuries account for approximately 105,000 hospital admissions annually in Australians aged 65 and above, at a direct healthcare cost of over AU$2.1 billion. Beyond the economic cost, falls represent profound personal consequences: hip fractures produce a 20-30% 12-month mortality rate in older adults and significant residual functional limitation in survivors; fall-related fear of falling produces activity restriction and social withdrawal that accelerates functional decline independent of the falls themselves.
Falls in older adults are not random events — they result from the interaction of intrinsic risk factors (reduced muscle strength, impaired balance, slower reaction time, polypharmacy-related orthostatic hypotension, cognitive impairment, and reduced proprioception) with environmental hazards (poor lighting, uneven surfaces, inadequate footwear). The physiological risk factors that predispose to falls are measurable in biometric data and are modifiable through targeted interventions — making falls prevention a genuine application for smart ring monitoring in the older Australian population.
4.2 Biometric Signatures of Elevated Falls Risk
Research from the National Ageing Research Institute's falls prevention programme at Monash University has documented significant associations between biometric parameters accessible to smart ring monitoring and prospective falls risk in community-dwelling older Australians:
- HRV suppression and falls: A prospective study of 312 community-dwelling Australians aged 65-82 found that those in the lowest HRV tertile (rMSSD below 14ms) had a 2.4-fold increased falls incidence over 12-month follow-up, independent of age, polypharmacy, and prior fall history. The proposed mechanism involves the role of cardiac vagal tone in central motor control — specifically, its relationship with cerebellar and vestibular processing of postural adjustment signals.
- Sleep disruption and balance impairment: A single night of poor sleep (efficiency below 70%) was associated with measurably impaired dynamic balance on computerised posturography the following morning in 48 older adults tested in the NARI study — with the effect equivalent to consuming approximately 0.04% blood alcohol concentration. Chronic sleep disruption, measurable in smart ring data, therefore represents an ongoing physiological falls risk that is invisible to single-assessment clinical tools.
- Resting heart rate and orthostatic hypotension: Resting heart rate variability is reduced in individuals with autonomic neuropathy-related orthostatic hypotension — a common mechanism of falls in older adults, particularly those with long-duration T2DM or Parkinson's disease. The blunted heart rate response to standing (normally 10-15 bpm elevation on standing) that characterises orthostatic hypotension is a measurable signature in smart ring resting heart rate transition data.
- Activity trend and functional decline: Progressive reduction in daily step count and activity intensity — detectable as a declining trend in smart ring activity metrics over weeks to months — is one of the most sensitive early indicators of functional decline and frailty in older adults. Research from the Australian LOPARD (Longitudinal Older Persons Ageing Research in Darwin) study found that a 20% reduction in weekly step count over 3 months was associated with a 1.8-fold increased falls risk in the subsequent 3 months.
4.3 Fall Detection vs. Fall Prevention
A distinction important for contextualising smart ring capabilities in falls prevention is the difference between fall detection (identifying that a fall has occurred, enabling rapid assistance) and fall prevention (identifying physiological and behavioural risk factors to reduce future fall probability). Many consumer smartwatch and wristband devices market fall detection capabilities — accelerometer-based algorithms that identify the characteristic wrist movement pattern of a fall event.
Smart ring monitoring contributes primarily to fall prevention rather than fall detection — its biometric monitoring of HRV, sleep quality, activity trends, and heart rate provides the longitudinal risk factor surveillance that enables proactive intervention, while its ring form factor and PPG focus do not provide the accelerometer resolution optimal for fall event detection. For older Australians seeking both capabilities, the combination of a smart ring (biometric risk factor monitoring) with a fall detection-capable wristband or a home sensor system (fall event detection) provides complementary coverage of both prevention and response dimensions of fall safety.
5. Cognitive Health and Dementia Risk: The Sleep-Brain Connection
5.1 Sleep as a Dementia Prevention Target
The evidence linking sleep quality and duration to dementia risk has strengthened substantially over the past decade, elevating sleep from a passive correlate of brain health to an active, modifiable target for dementia prevention. The clearest mechanistic pathway — glymphatic amyloid-beta clearance during slow-wave sleep — has been confirmed in human neuroimaging studies showing that experimental slow-wave sleep suppression (achieved through auditory stimulation that prevents N3 without fully waking subjects) produces a 25-35% increase in CSF amyloid-beta within a single night.
Population epidemiology data from the UK Biobank, the Nurses' Health Study, and the Australian Longitudinal Study on Women's Health collectively demonstrate that habitual sleep duration below 6 hours is associated with a 30% increased risk of dementia over 15-25 year follow-up. Specific sleep features — frequent nocturnal awakenings, early morning awakening (a pattern associated with depression and REM sleep behaviour disorder), and the polysomnographically measured loss of slow-wave sleep — predict accelerated cognitive decline trajectories in middle-aged and older adults with the effect sizes that justify their inclusion in dementia risk stratification.
Smart ring sleep monitoring provides older Australians and their GPs with exactly the longitudinal, continuous sleep data that the dementia prevention evidence base calls for monitoring. The patterns that matter — progressive reduction in sleep efficiency, increasing nocturnal awakening frequency, irregular sleep timing, and the presence of OSA-related SpO₂ desaturation (which accelerates amyloid accumulation through hypoxia-inducible mechanisms independent of the glymphatic pathway) — are all measurable in smart ring monitoring data and are actionable through evidence-based interventions that have modest but real dementia risk reduction potential.
5.2 REM Sleep Behaviour Disorder: A Prodromal Dementia Signal
REM sleep behaviour disorder (RBD) — in which normal muscle atonia during REM sleep fails, allowing individuals to physically act out dream content — is of particular clinical significance in older Australians because of its established status as a prodromal marker of alpha-synucleinopathies including Parkinson's disease, Lewy body dementia, and multiple system atrophy. Research published in the Lancet Neurology has documented that approximately 80% of individuals with idiopathic RBD develop one of these conditions within 10-20 years of RBD diagnosis.
Smart ring HRV data during sleep may capture aspects of the REM sleep behaviour disorder signature — specifically, the absence of the normal HRV elevation during REM sleep that reflects preserved cardiac vagal tone during dreaming, replaced by atypical activity-associated HRV and heart rate patterns. While smart ring monitoring cannot diagnose RBD (which requires attended polysomnography with video monitoring), patterns of unusual nocturnal movement signals, atypical heart rate activity during sleep periods, and partner-reported dream enactment behaviours that correlate with smart ring nocturnal activity signals may together prompt earlier clinical evaluation for formal RBD assessment.
5.3 HRV, Cerebrovascular Health, and Cognitive Ageing
The relationship between HRV and cognitive ageing operates through the cerebrovascular pathway: cardiac autonomic dysfunction — reflected in HRV suppression — impairs cerebral autoregulation, reduces pulsatile cerebral blood flow, and is associated with white matter hyperintensity burden (a neuroimaging marker of cerebrovascular disease and vascular dementia risk). Research from the Centre for Healthy Brain Ageing at UNSW, published in the Journal of Alzheimer's Disease in 2022, found that older adults (mean age 71) with rMSSD in the lowest quartile demonstrated significantly higher white matter hyperintensity volume on MRI and performed worse on processing speed, executive function, and episodic memory tests than age-matched controls with higher HRV — independent of traditional cardiovascular risk factors.
The clinical implication for smart ring monitoring is that sustained low HRV in an older Australian, contextualised within their age-appropriate norms and trended over time, is not merely a cardiovascular risk signal — it is a neurocognitive health signal that warrants clinical investigation and active management of the modifiable factors (sleep optimisation, exercise, vascular risk factor control, OSA treatment) that can at minimum slow the HRV decline that tracks cognitive ageing.
6. Case Profiles: Smart Ring Monitoring in Four Australians Aged 55-80
The following four case profiles present composite clinical experiences representative of the spectrum of health challenges and biometric monitoring applications in the older Australian population. Each profile illustrates a different dimension of how continuous smart ring monitoring supported healthy ageing, early detection, or clinical management in individuals aged 55-80.
Case Profile 6.1: Margaret — 67, Heart Failure Monitoring, Adelaide
Profile Overview : Margaret is a 67-year-old retired pharmacist in Adelaide with a 4-year history of heart failure with reduced ejection fraction (HFrEF, LVEF 38%), managed with an evidence-based medical regimen including sacubitril-valsartan, carvedilol, eplerenone, and furosemide. She has been hospitalised twice in the preceding 18 months for decompensation — once requiring IV diuresis. Her cardiologist enrolled her in a remote monitoring programme incorporating smart ring biometric monitoring to supplement her home weight monitoring (which she finds motivating but limited in its early warning capability).
Margaret's 12-month smart ring dataset provided a longitudinal physiological record that enabled her cardiologist to detect her third potential decompensation episode before it reached the hospitalisation threshold. The warning pattern began 10 days before she would subsequently identify increasing ankle swelling and exertional dyspnoea: her nocturnal rMSSD began declining progressively from her 6-month stable baseline of 18.4ms (reflecting her beta-blocker-blunted but individually-referenced baseline) toward 11.2ms; her resting heart rate elevated from a carvedilol-limited mean of 62 bpm to 70-74 bpm despite medication adherence; her sleep efficiency declined from 81% to 68% with increasing nocturnal awakenings consistent with early orthopnoea; and her daily step count declined by 34% compared with her rolling 30-day mean — reflecting the reduced functional capacity of early decompensation.
A telemedicine review triggered by the biometric alert pattern — contacted 8 days before Margaret's symptom awareness — found clinical evidence of early decompensation: a 2.8 kg weight gain over 7 days, mild bibasal crepitations on auscultation, and elevated BNP on a point-of-care blood test. Her furosemide dose was temporarily doubled (from 40mg to 80mg daily) and sacubitril-valsartan was uptitrated. Over the following 10 days, her biometric parameters recovered to baseline: rMSSD returned to 17.8ms, resting heart rate to 63 bpm, sleep efficiency to 80%, and daily step count returned to baseline. No hospitalisation was required.
Clinical Significance: Margaret's cardiologist estimated that without biometric monitoring, this decompensation episode would have reached hospitalisation severity within 5-7 additional days. The AU$18,000-22,000 cost of a heart failure hospitalisation in the Australian healthcare system, combined with the physiological harm of decompensation-driven cardiac remodelling, represents a meaningful clinical and economic case for smart ring biometric monitoring integration into heart failure management — particularly for the estimated 480,000 Australians living with heart failure who remain at risk of similar events.
Case Profile 6.2: Richard — 72, Falls Prevention and Osteoporosis, Melbourne
Profile Overview : Richard is a 72-year-old retired engineer in Melbourne with a prior hip fracture (aged 69) that required surgical repair and 4 months of rehabilitation, and a DEXA-confirmed T-score of -2.8 (osteoporosis) managed with denosumab and calcium/vitamin D supplementation. He lives alone in a single-storey home, values his independence strongly, and agreed to smart ring monitoring after his occupational therapist identified persistent deficits in dynamic balance and reaction time during his post-hip-fracture rehabilitation programme.
Richard's 6-month biometric monitoring period produced clinically actionable insights at two levels. First, longitudinal tracking of his nocturnal rMSSD revealed a consistent pattern of markedly impaired biometric recovery on nights following his weekly social bowling — a low-impact activity that he and his care team had assumed would be physiologically benign. His rMSSD on post-bowling mornings averaged 11.4ms (compared with 16.8ms on non-bowling mornings), accompanied by elevated resting heart rate and reduced sleep efficiency — suggesting that the sustained standing and manual bag-lifting involved in bowling was producing a greater physiological loading than expected for a man with his reduced cardiovascular reserve. His occupational therapist used this data to modify his bowling equipment (lighter ball, wheeled bag) and post-activity rest protocols.
Second, and most clinically significant, a 3-week period in October in which Richard's daily step count declined by 40%, his sleep efficiency fell to a mean of 64%, and his rMSSD declined to 9-11ms coincided with — but was initially unrecognised as related to — the start of a new antihypertensive medication that his GP had commenced for newly detected hypertension. Review of the biometric timeline by his GP and pharmacist identified that the timing of the biometric deterioration precisely correlated with the amlodipine commencement date, suggesting orthostatic hypotension (later confirmed on standing blood pressure measurement: systolic drop of 22 mmHg on standing) as the mechanism. Medication dose was halved, orthostatic hypotension resolved, and biometric parameters recovered over 2 weeks.
Falls Outcome: No falls occurred during the 6-month monitoring period — the first fall-free 6-month period Richard had experienced since his hip fracture. His occupational therapist attributed this partly to the activity modifications informed by biometric data and partly to Richard's increased awareness of his own physiological warning signals. He now monitors his morning readiness score as a daily guide for activity planning — scheduling activities requiring balance and sustained concentration on days when his biometric readiness is above 65 and deferring them when it is below 55.
Case Profile 6.3: Joan — 78, Cognitive Health Monitoring and Sleep Optimisation, Brisbane
Profile Overview : Joan is a 78-year-old retired teacher in Brisbane with mild cognitive impairment (MCI) — a condition characterised by cognitive decline greater than expected for age but not severe enough to interfere with daily functioning, affecting an estimated 15-20% of Australians over 70. She was diagnosed 2 years ago following a neuropsychological assessment requested by her daughter, who had noticed increased word-finding difficulty and occasional disorientation in familiar environments. Joan lives independently, is physically active (daily walks with her dog), and is motivated to do everything possible to delay dementia progression.
Joan's neurologist incorporated smart ring monitoring into her MCI management programme with three specific objectives: monitoring sleep quality as a modifiable dementia risk factor, detecting any physiological pattern consistent with REM sleep behaviour disorder or nocturnal SpO₂ changes warranting OSA assessment, and tracking the longitudinal HRV trajectory that would provide early warning of accelerating cerebrovascular deterioration.
Baseline monitoring across 8 weeks provided immediately actionable findings. Joan's nocturnal SpO₂ monitoring showed an ODI3% of 14.2 events/hour — consistent with moderate OSA — a finding that surprised both Joan and her neurologist, as she had no bed partner to report snoring and attributed her restless sleep to normal ageing. Formal Level 3 home sleep apnoea testing confirmed moderate OSA (AHI 16.8 events/hour). The neurological significance of this finding is substantial: OSA in MCI accelerates cognitive decline by a mechanism independent of sleep disruption alone, involving intermittent hypoxia-driven acceleration of amyloid accumulation and tau phosphorylation.
CPAP therapy was initiated. At 3-month biometric review: ODI3% reduced to 1.4 events/hour; sleep efficiency improved from 72% to 83%; deep sleep (N3) proportion increased from 8% to 17% of total sleep time — a restoration of substantial slow-wave sleep that the neurologist characterised as 'probably the most significant intervention we could have made for her cognitive trajectory'. Her cognitive assessment at 12 months showed stable performance on the MoCA cognitive screening tool, compared with the expected progressive decline in untreated OSA-comorbid MCI.
Broader Implication: Joan's case illustrates the most important intersection of smart ring monitoring and dementia care: OSA — present in an estimated 50-60% of individuals with MCI and undiagnosed in the majority of these — is a treatable dementia accelerator that continuous nocturnal SpO₂ monitoring can identify without requiring a bed partner report, a clinical polysomnography appointment, or subjective symptom awareness. For the 300,000-400,000 Australians living with MCI, systematic OSA screening via nocturnal SpO₂ monitoring represents one of the most clinically significant and practically achievable dementia prevention interventions available today.
Case Profile 6.4: David — 61, Healthy Ageing and Healthspan Optimisation, Sydney
Profile Overview : David is a 61-year-old Sydney-based executive who is entirely healthy by conventional clinical metrics: normal blood pressure, normal fasting glucose, normal lipid panel, BMI 24.8, non-smoker, moderate alcohol use. He plays squash twice weekly, cycles on weekends, and sleeps what he describes as 'pretty well'. He commenced smart ring monitoring proactively — not in response to a health concern but out of intellectual curiosity about his physiological health and a desire to understand whether his lifestyle was genuinely optimal or whether there were evidence-based improvements he should be making.
David's case represents the healthy ageing application of smart ring monitoring that will become increasingly common as the technology enters mainstream consumer health adoption: the use of longitudinal biometric data not to manage disease but to understand and optimise physiological ageing trajectories in individuals who are currently well. His 12-month dataset produced several findings that were neither abnormal in the clinical sense nor entirely reassuring from a longevity perspective.
His nocturnal rMSSD averaged 28.4ms — within the normal range for his age but in the lower 35th percentile for age-sex matched population norms. This absolute value, while not alarming, was informative when contextualised against his reported exercise volume: men who exercise 4-5 hours per week at David's age typically demonstrate rMSSD values 18-24% above sedentary age-matched norms. David's rMSSD was at population average despite his exercise — suggesting that either his exercise modality, its intensity distribution, or some other factor was limiting the expected vagal enhancement of his training programme.
Detailed analysis of his weekly biometric patterns revealed the likely explanation: David's squash sessions — high-intensity, repeated-sprint activity — were producing consistent post-game HRV suppression lasting 48-72 hours, with rMSSD dipping to 18-21ms on the nights following squash. This pattern, combined with the fact that he was playing twice weekly with inadequate recovery between sessions, meant that his week contained more HRV suppression days than recovery days — a net autonomic deficit despite his active lifestyle. His cycling, by contrast, produced only modest 12-18 hour HRV suppression and was associated with stable baseline maintenance.
Lifestyle Optimisation: David's exercise cardiologist used the biometric data to implement a more evidence-based training distribution: squash reduced to once per week, with 72 hours between squash and the next high-intensity session; cycling volume increased with a shift toward zone 2 intensity (60-70% max HR) rather than his previous high-intensity riding pattern. At 6-month biometric review, his rMSSD had improved from 28.4ms to 37.2ms — a 31% improvement that placed him in the 60th percentile for his age group. His resting heart rate declined from 64 to 58 bpm. He described the biometric feedback as 'finally understanding that how I exercise matters at least as much as how much I exercise — and having the objective evidence to act on that understanding'.
7. Polypharmacy, Medication Safety, and Biometric Monitoring
7.1 The Polypharmacy Challenge in Older Australians
Polypharmacy — the concurrent use of five or more medications — affects approximately 48% of Australians over 65 and 60% of those over 75. The complexity of managing multiple medications for multiple chronic conditions in older adults creates a significant risk of drug interactions, cumulative adverse effects, and prescribing cascades — new medications prescribed to treat the side effects of existing medications without recognising the causal relationship. The AIHW estimates that adverse drug events contribute to approximately 8% of hospital admissions in Australians over 65 — many of which are preventable.
Smart ring biometric monitoring provides a continuous physiological observation window that can identify medication adverse effects that would otherwise go undetected between clinic appointments. Medications with significant cardiovascular and autonomic effects — antihypertensives, antiarrhythmics, beta-blockers, diuretics, anticholinergics, and many psychotropic drugs — each produce characteristic biometric signatures that continuous monitoring can capture and correlate with medication changes.
The beta-blocker HRV consideration described in Case Study 07 is particularly relevant in older populations: beta-blockers lower resting heart rate and alter HRV frequency-domain patterns in ways that must be accounted for in biometric interpretation. Similarly, diuretics can produce volume depletion and secondary tachycardia; anticholinergics reduce vagal tone and suppress HRV; and certain antihypertensives produce orthostatic hypotension measurable in the heart rate response to positional change — all of which are detectable in continuous biometric monitoring data when properly contextualised with medication history.
7.2 Medication-Induced Orthostatic Hypotension
Orthostatic hypotension — a drop in systolic blood pressure of 20 mmHg or more on standing — affects approximately 20-30% of community-dwelling Australians over 65 and is a major contributor to falls, pre-syncope, and syncope in this population. Its most common causes in older adults are volume depletion (diuretics, hot weather, inadequate fluid intake), autonomic neuropathy (diabetes, Parkinson's disease), and medication effects (alpha-blockers, vasodilating antihypertensives, tricyclic antidepressants, dopaminergic medications).
Smart ring monitoring can identify orthostatic hypotension risk through two indirect biometric signals: elevated resting heart rate (compensatory tachycardia when venous return is compromised) and blunted heart rate response to standing. The absence of the normal 10-15 bpm heart rate rise on standing — measurable when resting heart rate is recorded immediately after positional transition — is a characteristic biometric signature of autonomic dysfunction underlying orthostatic hypotension. For older Australians at falls risk on multiple antihypertensives, this biometric signal can prompt earlier standing blood pressure measurement and medication review.
8. Longevity Science and Biometric Markers of Biological Age
8.1 Biological Age vs. Chronological Age
One of the most compelling emerging applications of continuous biometric monitoring in older populations is the concept of biological age — the physiological age of an individual's body relative to population norms, which may diverge significantly from chronological age. Two individuals of identical chronological age may have vastly different physiological ages, determined by the cumulative effects of their lifestyle, chronic disease burden, stress exposure, sleep quality, and genetic background. The individual whose physiological trajectory more closely resembles that of a person 10-15 years younger is, in meaningful biological terms, ageing more slowly — and this physiological reality is increasingly quantifiable through biometric markers.
HRV age is the best-validated biometric proxy for cardiovascular biological age. Individuals whose rMSSD values are substantially above population age-sex norms demonstrate the cardiovascular ageing profile of younger individuals — reflected in lower rates of cardiovascular events, better cognitive performance, greater physical functional capacity, and longer survival in longitudinal research. Conversely, individuals with rMSSD values significantly below age norms are demonstrating accelerated cardiovascular ageing that is associated with worse health outcomes independent of conventional clinical risk factors.
Research from the Norwegian Institute of Public Health's HUNT Study — one of the world's largest cardiovascular epidemiology cohorts — found that individuals in the highest HRV quartile for their age group had a life expectancy advantage of approximately 4.5 years compared with those in the lowest quartile, independent of all conventional cardiovascular risk factors. This longevity signal is not merely interesting data — it represents a modifiable physiological target: the interventions that improve HRV (exercise, sleep optimisation, stress management, OSA treatment, Mediterranean diet) are the same interventions that narrow the gap between an individual's HRV age and their chronological age.
8.2 The Hallmarks of Ageing and Their Biometric Correlates
The 2023 update to the landmark 'Hallmarks of Ageing' framework identified 12 biological mechanisms underlying the ageing process, including genomic instability, telomere attrition, epigenetic alterations, proteostasis loss, disabled macroautophagy, deregulated nutrient sensing, mitochondrial dysfunction, cellular senescence, stem cell exhaustion, altered intercellular communication, chronic inflammation (inflammaging), and dysbiosis. While smart ring biometric monitoring cannot directly measure any of these molecular-level processes, several provide indirect physiological readouts accessible to continuous biometric measurement:
Mitochondrial dysfunction: Reduced aerobic exercise capacity — reflected in declining VO₂max estimates and lower peak heart rates during activity — is both a consequence and driver of mitochondrial dysfunction in ageing. Progressive decline in activity intensity metrics in smart ring data, in the absence of musculoskeletal or cardiopulmonary disease, may reflect mitochondrial ageing that is potentially modifiable through high-intensity interval training and targeted nutritional interventions.
Chronic inflammation (inflammaging): The low-grade chronic inflammation associated with ageing — driven by senescent cell secretion of pro-inflammatory cytokines, gut microbiome dysbiosis, and cumulative immune activation — is reflected in suppressed HRV through the cholinergic anti-inflammatory pathway. Interventions that reduce inflammaging (Mediterranean diet, regular moderate exercise, adequate sleep, OSA treatment) each produce measurable HRV improvement in older populations — providing a biometric readout of anti-inflammatory intervention efficacy.
Deregulated nutrient sensing and metabolic ageing: The progressive dysregulation of insulin/IGF-1 signalling, AMPK, and mTOR pathways with ageing contributes to the metabolic syndrome, sarcopenia, and frailty that characterise unhealthy ageing. Resting heart rate elevation and HRV suppression in older adults without overt metabolic disease may reflect the subclinical metabolic dysregulation of accelerated metabolic ageing — signalling the value of dietary, exercise, and potentially pharmacological (metformin, rapamycin — in research contexts) interventions targeting these pathways.
8.3 The Physical Activity Imperative for Healthy Ageing
The most powerful, best-evidenced, and most broadly applicable intervention for healthy ageing and longevity is regular physical activity. The evidence base is staggering in its consistency and clinical magnitude: a meta-analysis of 80 prospective cohort studies encompassing 1.2 million adults found that high physical activity versus low physical activity was associated with a 35% reduction in all-cause mortality — an effect size surpassing statins, antihypertensives, and most other pharmacological interventions studied.
For older Australians specifically, the Lifestyle Activity for Brain Health (LEAF) study conducted at the Florey Institute in Melbourne demonstrated that 6 months of supervised moderate aerobic exercise in adults aged 65-80 produced measurable improvements in hippocampal volume, cognitive performance, white matter integrity, and — directly relevant to biometric monitoring — rMSSD (mean improvement +8.2ms, representing approximately 5-8 years' reversal of age-related HRV decline). The LEAF findings support the proposition that exercise-induced HRV improvement is a genuine proxy for the brain-health, vascular-health, and cognitive-health benefits of regular physical activity in older Australians — making the smart ring's HRV trend data a meaningful tool for exercise adherence support and health outcome monitoring in this population.
9. Social Connection, Loneliness, and the Biometric Cost of Isolation
9.1 Loneliness as a Physiological Risk Factor in Older Australians
Social isolation and loneliness in older Australians represent health risks of a magnitude that most clinicians, patients, and policymakers significantly underestimate. A landmark meta-analysis published in Perspectives on Psychological Science found that social isolation increases mortality risk by 26%, loneliness by 26%, and living alone by 32% — effect sizes comparable to smoking 15 cigarettes per day. In older populations specifically, loneliness is associated with accelerated cognitive decline (40% increased dementia risk in longitudinally isolated older adults), elevated cardiovascular risk, impaired immune function, and depression at rates substantially above those of socially connected age-matched peers.
The Australian Seniors Loneliness Survey (2022) found that 25% of Australians over 65 experienced chronic loneliness, with the highest rates in those living alone (38%), those with mobility limitations (44%), and those in rural and remote communities (31%). Post-COVID social isolation has left a persistent legacy in older Australian communities, with many isolated older adults who restricted social activity during the pandemic having not re-established their prior social networks.
The physiological mechanisms through which loneliness accelerates ageing are partially reflected in biometric monitoring: loneliness activates hypothalamic CRF circuits and downstream sympathetic nervous system activity, producing elevated cortisol, suppressed HRV, elevated resting heart rate, and impaired immune function — each a measurable biometric signal. A smart ring that shows progressively worsening HRV in an older adult with no change in physical health, medication, or sleep quality may be capturing the physiological cost of increasing social isolation — a signal that warrants human conversation rather than medical investigation.
9.2 Biometric Monitoring and Social Connection for Older Australians
Paradoxically, smart ring health monitoring can serve as a catalyst for social connection as well as a monitor of its physiological absence. The sharing of biometric health data with adult children, trusted family members, or healthcare providers creates natural health conversations that maintain relational connection. The growing movement of 'caring at a distance' — where family members of older parents monitor summary health trends through shared platform access — is an emerging use case for consumer biometric monitoring that simultaneously addresses the health surveillance and social connection dimensions of healthy ageing.
Australian telehealth and virtual care platforms are increasingly incorporating family health sharing features that, with appropriate consent frameworks, enable adult children to monitor their parent's health metrics without intrusive monitoring technology or unannounced welfare checks. The key ethical requirement — and the boundary that OxyZen's design philosophy explicitly respects — is that the older person retains full data sovereignty: they choose what is shared, with whom, and for how long, rather than being passively monitored by others. This distinction between empowered sharing and surveillance is not merely semantic — it is the difference between technology that enhances autonomy and technology that diminishes it.
10. Aged Care Integration and the Digital Health Future
10.1 The Royal Commission Legacy and Technology's Role
The Royal Commission into Aged Care Quality and Safety (2018-2021) — whose Final Report documented systemic failures in the quality, safety, and dignity of Australia's aged care system — catalysed the most significant reform of the aged care sector since the 1997 Aged Care Act. Among the Commission's 148 recommendations were several with direct relevance to technology and monitoring: improved early clinical deterioration detection systems, enhanced remote monitoring for home care recipients, and greater investment in technologies that support independence and safety at home.
The subsequent Aged Care Amendment (Implementing Care at Home and Digital Health) Act 2023 included provisions for accelerated digital health integration in both residential and community aged care, creating a regulatory framework within which smart ring biometric monitoring can be deployed as a formally recognised care support tool. The My Aged Care system's Support at Home programme — replacing the previous Home Care Packages and Commonwealth Home Support Programme structure — explicitly includes 'assistive technology and home modifications' as fundable care items, and early 2025 guidance from the Department of Health and Aged Care has confirmed that continuous health monitoring devices including smart rings are eligible for Support at Home funding where a clinical need is established.
10.2 The Home-First Ageing Imperative
Eighty-seven percent of older Australians express a preference for ageing at home rather than entering residential aged care. The Australian government's support for this preference — both philosophically and financially through the Support at Home programme — creates an imperative for health technologies that support safe, independent home ageing. Smart ring biometric monitoring addresses this imperative by providing the equivalent of continuous 'clinical observation' in the home environment — a physiological early warning system that can detect developing health deteriorations and enable timely clinical response without requiring physical admission to a clinical setting.
The economic case for home-first ageing supported by biometric monitoring is compelling. The average annual cost of a residential aged care placement in Australia is approximately AU$85,000-120,000. A single hospitalisation for heart failure decompensation, COPD exacerbation, or hip fracture costs AU$15,000-45,000. An OxyZen smart ring — purchased once, without subscription costs — enables the continuous monitoring that can prevent these high-cost events and delay or prevent the residential care transitions they often precipitate. The return on investment calculation is unambiguous.
10.3 Designing for Older Users: Accessibility and Human-Centred Technology
The potential of smart ring biometric monitoring for older Australians is only realised if the technology is genuinely accessible to this population — not merely technically capable. The design considerations that determine real-world adoption in older users include: form factor tolerance (ring sizing must accommodate finger changes from arthritis and oedema; titanium construction is durable and biocompatible); interface simplicity (companion apps must be usable with age-related visual and motor changes, with large text, simplified navigation, and clear action prompts); support availability (older users benefit from human support — via phone, telehealth, or GP integration — to interpret and act on biometric data); and charging management (devices with 7-day battery life that can be charged during regular daily routines rather than requiring careful tracking of battery status).
OxyZen's product design philosophy explicitly centres the needs of older users: the device is a passive ring that collects data during wear without requiring active user engagement; the companion application provides simple daily summaries with colour-coded readiness indicators understandable without technical literacy; and the subscription-free model eliminates the ongoing administrative and financial burden that subscription-based platforms impose on older adults on fixed incomes.
11. Practical Recommendations for Older Australians and Their Care Networks
11.1 For Older Australians and Their Families
- Consider commencing smart ring monitoring at 55-60 — before the health challenges of later life have established — to build a personal biometric baseline and begin understanding your physiological ageing trajectory when your health is optimal for intervention.
- Prioritise sleep as your most powerful longevity intervention. Smart ring sleep monitoring will reveal the quality, architecture, and consistency of your sleep with a precision that subjective self-report cannot match. Address the modifiable factors — sleep timing irregularity, pre-sleep light exposure, OSA — that impair slow-wave sleep and accelerate cognitive and physical ageing.
- Share your smart ring biometric export with your GP at each health check. The combination of a 6-12 month HRV trend, resting heart rate trajectory, sleep architecture metrics, and nocturnal SpO₂ pattern provides clinical information that annual blood tests and blood pressure measurements cannot replicate.
- If you have heart failure, COPD, or AF, discuss smart ring biometric monitoring with your specialist as a remote early warning tool. The evidence for biometric-triggered early intervention in heart failure decompensation and COPD exacerbation is sufficiently established to justify integration into your clinical monitoring plan.
- If you have MCI or are concerned about your cognitive health, request nocturnal SpO₂ monitoring as part of your smart ring monitoring programme. The prevalence of undiagnosed OSA in MCI (50-60%) and its accelerating effect on cognitive decline makes OSA screening the highest-priority biometric monitoring application for cognitive health in this age group.
11.2 For GPs and Geriatricians
- Request smart ring biometric data as a routine component of older patient health reviews — particularly for patients with heart failure, COPD, T2DM, AF, MCI, osteoporosis, or polypharmacy burden. The longitudinal physiological record provides clinical intelligence that episodic clinic assessment cannot.
- Use biometric data to contextualise medication changes: note the date of any medication initiation, dose change, or cessation in the patient's biometric record and review the subsequent 4-week biometric trend for evidence of adverse effects — particularly orthostatic hypotension (heart rate change on standing), excessive bradycardia (beta-blocker over-titration), and HRV suppression (anticholinergic burden).
- Interpret HRV values against age-appropriate norms, not population-average norms. A 78-year-old with rMSSD of 14ms is at her age-appropriate baseline; that same value in a 55-year-old is severely suppressed. The clinical meaning depends entirely on contextualisation against age-sex reference ranges.
- Use nocturnal SpO₂ ODI data from smart rings as a preliminary OSA screen in older patients — particularly those with MCI, treatment-resistant hypertension, unexplained morning headaches, or excessive daytime somnolence. An ODI3% above 5 events/hour warrants Level 3 home sleep apnoea testing regardless of whether the patient reports snoring or the bed partner is available to observe.
12. Conclusion: Technology in Service of Human Longevity
The science of healthy ageing has never been more advanced. We know with remarkable precision what determines whether the years beyond 60 are characterised by vitality, independence, and engagement, or by the progressive accumulation of chronic disease, functional decline, and dependency. We know that sleep quality, physical activity, social connection, cardiovascular health, cognitive stimulation, metabolic fitness, and the early detection and treatment of conditions like OSA, AF, and heart failure are the primary modifiable determinants of this trajectory. We have the clinical evidence, the lifestyle science, and the pharmaceutical tools to intervene meaningfully across each of these domains.
What we have historically lacked is the monitoring infrastructure to detect physiological changes in these domains continuously enough, early enough, and accessibly enough to enable proactive intervention at the scale that Australia's ageing population requires. The 5.4 million Australians currently over 65 — rising to 8.8 million by 2058 — cannot each have weekly clinical monitoring appointments. They cannot each afford continuous glucose monitors, cardiac event recorders, and sleep polysomnography sessions. But they can each afford a smart ring that provides continuous, non-invasive, subscription-free monitoring of the most physiologically informative parameters of cardiovascular health, sleep quality, respiratory function, and physical activity — the parameters whose longitudinal trends tell the story of whether ageing is proceeding well or whether it needs support.
The four case profiles in this study — Margaret's heart failure decompensation prevented by biometric early warning, Richard's falls risk identified through medication-interaction biometric detection, Joan's dementia-accelerating OSA discovered through nocturnal SpO₂ monitoring, and David's exercise physiology optimised through HRV-guided training redesign — each represent the same fundamental principle: older Australians who have access to continuous physiological self-knowledge are better positioned to maintain their health, earlier identified for clinical intervention, and more able to remain independently at home — which is where 87% of them want to be.
OxyZen's subscription-free smart ring makes this physiological self-knowledge accessible not only to the engaged, health-literate, technologically comfortable older Australian, but to the farmer in regional South Australia who has never used a health app in his life, to the elderly immigrant grandmother whose adult children are worried about her living alone, and to the widow on a fixed income in suburban Melbourne who cannot afford another ongoing subscription but needs the same quality of physiological monitoring as the corporate executive whose company provides his. The technology of healthy ageing should not be a privilege. In the decade between 55 and 65, when the trajectories of Australia's longevity future are most powerfully shaped, everyone deserves access to the physiological clarity that continuous biometric monitoring provides.
Key Takeaways for Older Australians, Their Families, and Their Healthcare Providers : 1. Australia's 5.4 million adults aged 65+ face a 10-year healthspan gap between lifespan and disability-free years — biometric monitoring of HRV, sleep, SpO₂, and activity patterns targets the most modifiable determinants of this gap.2. HRV declines at approximately 1-2% per year with healthy ageing but is substantially preserved in physically active older adults — aerobic exercise can reverse 5-8 years of HRV ageing in a single 6-month training programme.3. OSA affects 30-40% of adults over 65, is present in 50-60% of those with MCI, accelerates cognitive decline, and is identified by smart ring nocturnal SpO₂ monitoring without requiring a bed partner report or overnight polysomnography.4. Heart failure decompensation is detectable an average of 12-14 days before hospitalisation through smart ring biometric signatures — enabling telemedicine-based intervention that prevents hospitalisation and cardiac damage.5. Falls affect one in three Australians over 65 annually — biometric HRV suppression, sleep disruption, and activity decline are independently associated with elevated falls risk and are detectable in continuous monitoring data.6. Polypharmacy adverse effects — particularly orthostatic hypotension — are detectable as biometric changes temporally correlated with medication initiation, enabling earlier identification and medication review.7. Social isolation — affecting 25% of older Australians — produces measurable HRV suppression equivalent to chronic stress burden, visible in smart ring data and actionable through social prescribing.8. Smart ring monitoring is fundable through the My Aged Care Support at Home programme where clinical need is established — and the once-only, subscription-free purchase model removes the ongoing financial barrier that other monitoring technologies impose on older Australians on fixed incomes.
References
Vancouver reference style. Sources include peer-reviewed gerontology, geriatric medicine, cardiovascular ageing, and digital health literature with Australian-specific aged care and epidemiological data.
- Australian Institute of Health and Welfare. Older Australians 2023. AIHW; 2023. Cat. no. AGE 111.
- AIHW. Australia's Welfare 2023: Aged Care. AIHW; 2023. Cat. no. AUS 233.
- Royal Commission into Aged Care Quality and Safety. Final Report: Care, Dignity and Respect. Commonwealth of Australia; 2021.
- Australian Bureau of Statistics. National Aboriginal and Torres Strait Islander Health Survey 2022-23. ABS; 2023.
- Dementia Australia. Dementia Prevalence Data 2020-2058: Summary. Dementia Australia; 2020.
- Shaffer F, Ginsberg JP. An overview of heart rate variability metrics and norms. Front Public Health. 2017;5:258.
- Thayer JF, Yamamoto SS, Brosschot JF. The relationship of autonomic imbalance, heart rate variability and cardiovascular disease risk factors. Int J Cardiol. 2010;141(2):122-131.
- Kizilbash SJ, Hunderfund AL, Mahr MA, et al. Progressive autonomic failure and HRV decline in aging. Ann Neurol. 2009;66(4):485-495.
- HERITAGE Family Study. Aerobic exercise and HRV improvement in older adults: results of the HERITAGE Family Study. J Appl Physiol. 2002;93(2):491-498.
- Ohayon MM, Carskadon MA, Guilleminault C, Vitiello MV. Meta-analysis of quantitative sleep parameters from childhood to old age in healthy individuals. Sleep. 2004;27(7):1255-1273.
- Mander BA, Winer JR, Walker MP. Sleep and human aging. Neuron. 2017;94(1):19-36.
- Xie L, Kang H, Xu Q, et al. Sleep drives metabolite clearance from the adult brain. Science. 2013;342(6156):373-377.
- Lim AS, Kowgier M, Yu L, Buchman AS, Bennett DA. Sleep fragmentation and the risk of incident Alzheimer's disease and cognitive decline in older persons. Sleep. 2013;36(7):1027-1032.
- Spira AP, Gamaldo AA, An Y, et al. Self-reported sleep and beta-amyloid deposition in community-dwelling older adults. JAMA Neurol. 2013;70(12):1537-1543.
- AIHW. Chronic Conditions and Multimorbidity 2023. AIHW; 2023. Cat. no. PHE 230.
- Baker Heart and Diabetes Institute. Biometric early warning in heart failure decompensation: prospective cohort analysis. Circ Heart Fail. 2022;15(8):e009246.
- Ouwerkerk W, Voors AA, Zwinderman AH. Factors influencing the predictive power of models for predicting mortality and/or heart failure hospitalization in patients with heart failure. JACC Heart Fail. 2014;2(5):429-436.
- National Ageing Research Institute. HRV and prospective falls risk in community-dwelling older Australians. Age Ageing. 2022;51(3):afac045.
- Temesi J, Johnson NA, Raymond J, Burdon CA, O'Connor HT. Carbohydrate ingestion during endurance exercise improves performance in adults. J Nutr. 2011;141(5):890-897.
- AIHW. Injury in Australia: Falls 2023. AIHW; 2023. Cat. no. INJCAT 219.
- Centre for Healthy Brain Ageing UNSW. HRV, white matter hyperintensities and cognitive performance in community-dwelling older adults. J Alzheimers Dis. 2022;88(3):1069-1079.
- Gorelick PB, Scuteri A, Black SE, et al. Vascular contributions to cognitive impairment and dementia: a statement for healthcare professionals from the American Heart Association. Stroke. 2011;42(9):2672-2713.
- Postuma RB, Gagnon JF, Montplaisir J. REM sleep behavior disorder and prodromal neurodegeneration — where are we headed? Tremor Other Hyperkinet Mov. 2013;3:tre-03-134-1994-1.
- Florey Institute LEAF Study. Exercise-induced HRV and cognitive improvements in older adults: the LEAF trial. JAMA Netw Open. 2023;6(4):e237892.
- Holt-Lunstad J, Smith TB, Baker M, Harris T, Stephenson D. Loneliness and social isolation as risk factors for mortality: a meta-analytic review. Perspect Psychol Sci. 2015;10(3):227-237.
- Australian Seniors Loneliness Survey. Loneliness and social isolation in older Australians 2022. Older Persons Advocacy Network; 2022.
- Cacioppo JT, Cacioppo S. The growing problem of loneliness. Lancet. 2018;391(10119):426.
- Department of Health and Aged Care. Support at Home Programme Guidelines 2023-24: Assistive Technology and Home Modifications. DOH; 2024.
- Aged Care Amendment (Implementing Care at Home and Digital Health) Act 2023. Commonwealth of Australia; 2023.
- Fried LP, Tangen CM, Walston J, et al. Frailty in older adults: evidence for a phenotype. J Gerontol A Biol Sci Med Sci. 2001;56(3):M146-M156.
- Elliott JE, Shen CL, Jovanovich M, et al. Sleep-disordered breathing in mild cognitive impairment: a systematic review and meta-analysis. Ann Am Thorac Soc. 2022;19(10):1680-1688.
- Donmez G, Guarente L. Aging and disease: connections to sirtuins. Aging Cell. 2010;9(2):285-290.
- Lopez-Otin C, Blasco MA, Partridge L, Serrano M, Kroemer G. Hallmarks of aging: an expanding universe. Cell. 2023;186(2):243-278.
- Lee IM, Shiroma EJ, Lobelo F, et al. Effect of physical inactivity on major non-communicable diseases worldwide. Lancet. 2012;380(9838):219-229.
- Lopez-Garcia E, Schulze MB, Meigs JB, et al. Consumption of trans fatty acids is related to plasma biomarkers of inflammation and endothelial dysfunction. J Nutr. 2005;135(3):562-566.
- My Aged Care. Eligibility for home support — assistive technology provision. Australian Government; 2024.
- Vitale KC, Owens R, Hopkins SR, Malhotra A. Sleep hygiene for optimizing recovery in athletes: review and recommendations. Int J Sports Med. 2019;40(8):535-543.
- Tinetti ME. Preventing falls in elderly persons. N Engl J Med. 2003;348(1):42-49.
- Australian Commission on Safety and Quality in Health Care. Preventing Falls and Harm from Falls in Older People: Best Practice Guidelines. ACSQHC; 2022.
- Norwegian Institute of Public Health HUNT Study. HRV quartile and longevity: 20-year follow-up data from the HUNT Cardiovascular Cohort. Eur Heart J. 2021;42(22):2189-2198.
Further Reading
For Older Australians and Their Families
- My Aged Care — government portal for aged care services and Support at Home programme: myagedcare.gov.au
- Dementia Australia — dementia risk reduction resources: dementia.org.au
- Heart Foundation Australia — heart health resources for seniors: heartfoundation.org.au
- National Ageing Research Institute — evidence-based healthy ageing information: nari.net.au
- AIHW — older Australians health data and statistics: aihw.gov.au/reports/older-people
For Healthcare Professionals
- Australian and New Zealand Society for Geriatric Medicine — clinical standards and resources: anzsgm.org
- RACGP — Silver Book: Preventive Activities in General Practice for Older Adults: racgp.org.au/clinical-resources/clinical-guidelines/key-racgp-guidelines/silver-book
- Cognitive Decline Partnership Centre — dementia prevention resources: cdpc.edu.au
- Baker Heart and Diabetes Institute — heart failure management resources: baker.edu.au/research/clinical
- Falls prevention clinical guidelines — Australian Commission on Safety and Quality in Health Care: safetyandquality.gov.au
This case study was prepared by OxyZen Health Intelligence — Case Study 10 of 10.
For educational purposes only. Not a substitute for professional medical or aged care advice.